Accountable care organizations have major challenges integrating social services with medical care, including a lack of data on their patients’ social needs and the capabilities of community partners.
That’s the finding of a new study published in the journal Health Affairs, based on qualitative data from 22 ACOs.
“The ACOs in our sample frequently lacked data about several dimensions that could inform decision making and efforts to integrate social services and medical care, a phenomenon we characterize as the ACOs’ ‘flying blind’,” state the study’s authors. “At the most basic level, most ACOs lacked data on their own patients’ social needs.”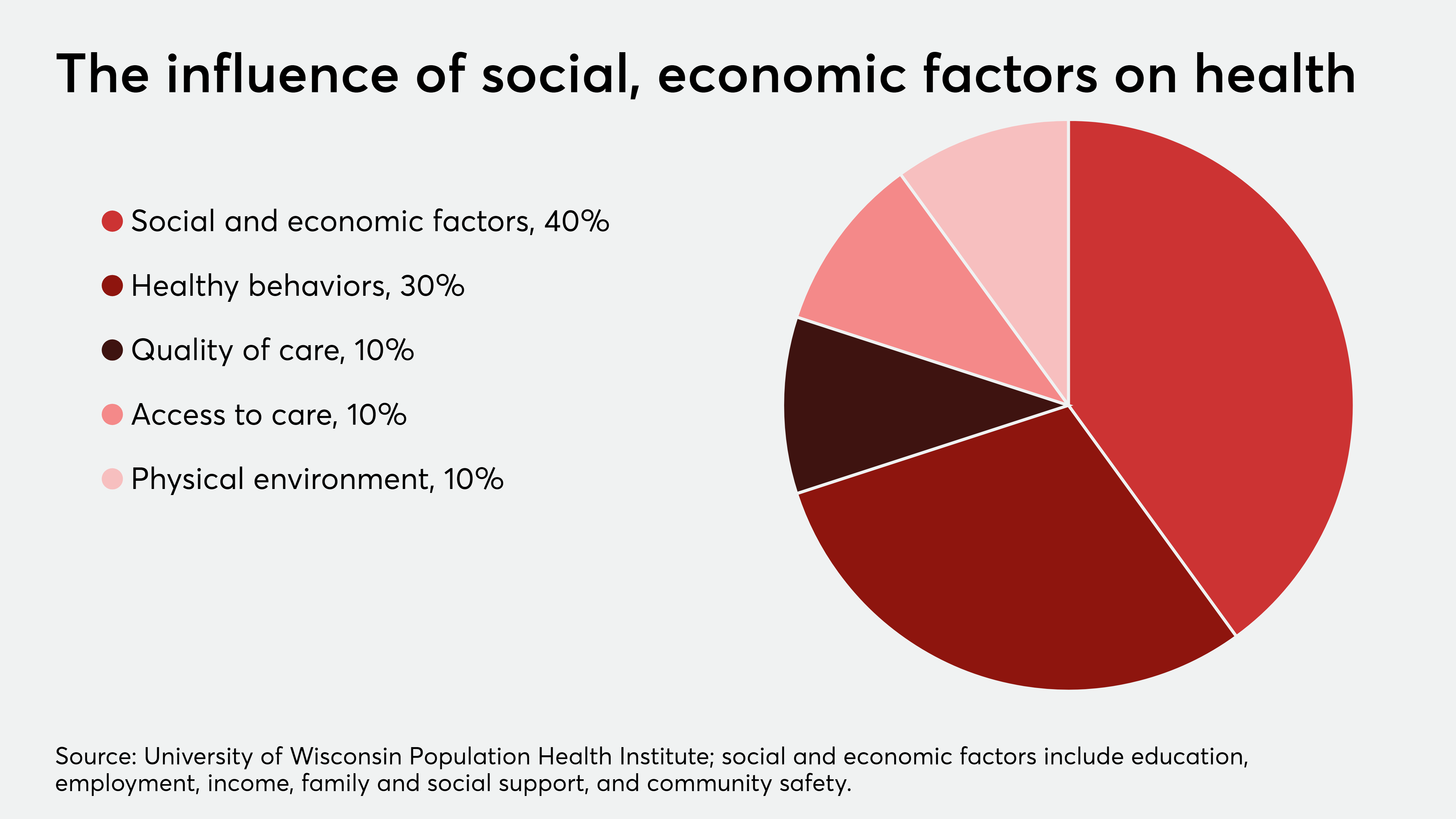
While ACOs in the study reported a strong interest in leveraging data and technology to better address social needs, for most of these organizations that is a future aspiration and not a current reality.
“Only half of the ACOs in our sample conducted standardized screening for social needs, and 45 percent used a standardized approach to documentation,” according to the study. “Moreover, even where standard screening was conducted, results were frequently not shared with relevant personnel across the ACO.”
In addition, ACOs lacked data on the quality of community-based organizations to use in developing and evaluating partnerships.
“When exploring partnerships with local community-based organizations, ACOs generally had no standard data to use in assessing the quality and capabilities of local providers,” state the authors. “Instead, respondents reported making informal assessments of potential community-based organization partners’ quality based on factors such the organization’s longevity, ACO leaders’ impressions from informational and informal meetings with local leaders of the community-based organization, and colleagues’ assessments of its organizational quality.”
The study also found that most ACOs were not exchanging any data with community partners after programs were developed.
“A minority of ACOs in our sample shared data with community partners, with only 14 percent planning to share and 9 percent currently sharing electronic data (such as data from EHRs),” according to the study. “Most were still struggling with internal clinical EHR interoperability and had not even begun to imagine sharing access with community partners.”
“Policies that could facilitate the integration of social determinants include providing sustainable funding, implementing local and regional networking initiatives to facilitate partnership development, and developing standardized data on community-based organizations’ services and quality to aid providers that seek partners,” says Genevra Murray, a research scientist at the Dartmouth Institute for Health Policy and Clinical Practice, who collaborated with colleagues from the University of California Berkeley and the University of North Carolina at Chapel Hill on the study.
